The current standard of care for OSA is continuous positive airway pressure (CPAP). Ninty percent of patients diagnosed with OSA are prescribed CPAP therapy [1], however compliance to CPAP is poor with 46% to 83% of patients non-compliance. [2, 3]. Effectiveness of CPAP is potentially high, but observed at only 50%. [4]
The lack of CPAP compliance has created a large unmet clinical need that must offer:
- better compliance
- low morbidity – fewer related diseases and medical conditions
- consistent effectiveness
Overview of treatment options
Weight Loss and Positional Therapy
 About 70% of people with Obstructive Sleep Apnea (OSA) are overweight or obese. Their healthcare providers typically encourage them to lose weight and/or to use positional therapy as part of a first line of treatment. Some people can eliminate or reduce airway blockage by sleeping on their side versus their back.
About 70% of people with Obstructive Sleep Apnea (OSA) are overweight or obese. Their healthcare providers typically encourage them to lose weight and/or to use positional therapy as part of a first line of treatment. Some people can eliminate or reduce airway blockage by sleeping on their side versus their back.
Positional therapy generally works only in mild cases of OSA. In more severe cases, the airway collapses no matter the patient’s sleeping position.
CPAP
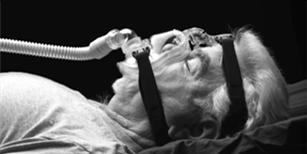 Continuous positive airway pressure (CPAP) therapy uses a machine with a tube and a mask to blow air into a person’s airways. The mask supplies pressurized air that flows continuously into the airways. The increased air pressure prevents the sleeper’s airway from collapsing. In addition to CPAP, there are several types of PAP machines. For example; BiPAP (bilevel positive airway pressure) and VPAP (variable positive airway pressure).
Continuous positive airway pressure (CPAP) therapy uses a machine with a tube and a mask to blow air into a person’s airways. The mask supplies pressurized air that flows continuously into the airways. The increased air pressure prevents the sleeper’s airway from collapsing. In addition to CPAP, there are several types of PAP machines. For example; BiPAP (bilevel positive airway pressure) and VPAP (variable positive airway pressure).
There are many challenges with CPAP compliance for a lot of patients. Patients can’t tolerate it or they don’t use it consistently, e.g. only a few hours a night and/or a few nights a week.
A variant on the PAP technology is EPAP, expiratory positive airway pressure. Using the same principal of keeping the lungs full and the upper airway open, this therapy is applied by a daily disposable valve, which is applied to each nostril before bed. Similar to CPAP this can be hard for patients to get used to due to the high pressures created in the airways.
Oral Appliances
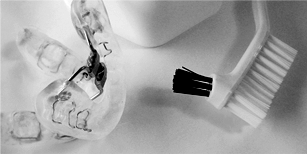 Oral appliances fit inside your mouth similar to an athletic mouth guard. Others fit around your head and chin to adjust the position of your lower jaw. Two common oral devices are the mandibular repositioning device and the tongue-retaining device. These devices open your airway by bringing your lower jaw or your tongue forward during sleep.
Oral appliances fit inside your mouth similar to an athletic mouth guard. Others fit around your head and chin to adjust the position of your lower jaw. Two common oral devices are the mandibular repositioning device and the tongue-retaining device. These devices open your airway by bringing your lower jaw or your tongue forward during sleep.
Some oral appliances are custom made and fitted by a dentist, others are sent directly to a person’s home to be fitted by the user.
Oral appliances are an option only for people with mild to moderate sleep apnea. Some people experience pain, teeth movement and jaw problems after continued use of oral appliances.
Surgery
 Surgery can be performed to improve the size or tone of a patient’s airway:
Surgery can be performed to improve the size or tone of a patient’s airway:
- Nasal surgery, including turbinectomy (removal or reduction of a nasal turbinate), or straightening of the nasal septum, in patients with nasal obstruction or congestion which reduces airway pressure and complicates OSA.
- Tonsillectomy and/or adenoidectomy in an attempt to increase the size of the airway.
- Removal or reduction of parts of the soft palate and some or all of the uvula, such as uvulopalatopharyngoplasty (UPPP) or laser-assisted uvulopalatoplasty (LAUP). Modern variants of this procedure sometimes use radiofrequency waves to heat and remove tissue.
- Reduction of the tongue base, either with laser excision or radiofrequency ablation.
- Genioglossus advancement, in which a small portion of the lower jaw that attaches to the tongue is moved forward, to pull the tongue away from the back of the airway.
- Hyoid suspension, in which the hyoid bone in the neck, another attachment point for tongue muscles, is pulled forward in front of the larynx.
- Maxillomandibular advancement (MMA), which moves the upper jaw (maxilla) and the lower jaw (mandible) forward. There is a longer recovery when compared to other sleep apnea surgeries, since the bones of the face have to heal into their new position.
Most of these surgical procedures are quite invasive and are associated with significant pain and recovery time. The procedures are not always successful in treating OSA.
The ReVENT® Sleep Apnea System
 The ReVENT Sleep Apnea System treats obstruction in patients with mild to severe OSA.
The ReVENT Sleep Apnea System treats obstruction in patients with mild to severe OSA.
The System can be used as a standalone therapy, or can be combined with some of the therapies listed above. The technology addresses the non-compliance issues inherent with CPAP therapy as well as the invasiveness and recovery time associated with surgical procedures for the treatment of OSA.
For additional information on the ReVENT Sleep Apnea System, click here.
- U.S. Sleep Apnea Diagnostic and Therapeutic Devices Markets, Frost&Sullivan, Editor. 2010.
- Kribbs, N.B., et al., Objective measurement of patterns of nasal CPAP use by patients with obstructive sleep apnea. Am Rev Respir Dis, 1993. 147(4): p. 887-95.
- Weaver, T.E. and R.R. Grunstein, Adherence to continuous positive airway pressure therapy: the challenge to effective treatment. Proc Am Thorac Soc, 2008. 5(2): p. 173-8.
- Grote, L., et al., Therapy with nCPAP: incomplete elimination of Sleep Related Breathing Disorder. Eur Respir J, 2000. 16(5): p. 921-7.

